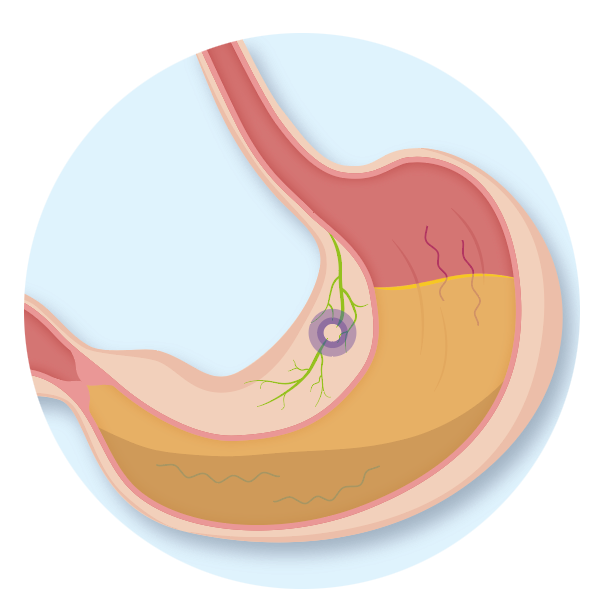

Gastroparesis is a long-term condition where the stomach cannot empty food and drink in the normal way. Food passes through the stomach more slowly than usual because certain nerves and muscles do not work properly. This can also be called delayed gastric emptying.
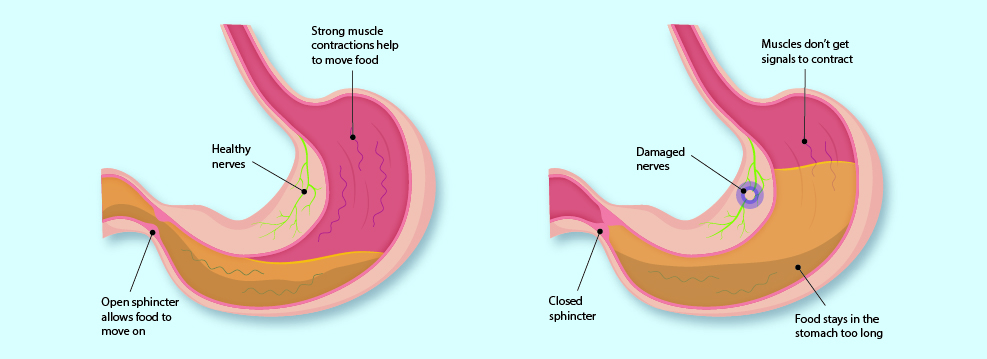
Common symptoms of gastroparesis include:

Eating differently may help the symptoms of gastroparesis. A dietitian can discuss changes that might help. The main goals are to:

The first thing to consider is eating smaller more frequent meals. Having 6-8 smaller meals throughout the day may help to reduce feelings of fullness and bloating. This can help you eat enough calories to meet your daily needs. Have drinks 30 minutes before or after meals, rather than with your meal, to avoid over filling the stomach. A 10 minute walk or other light activity after meals can also help digestion.

Foods that are high in fat slow down stomach emptying and may make your symptoms worse. Experiment by choosing foods that are lower in fat to see if they improve your symptoms. However, many people with gastroparesis have no trouble with fats in drinks such as, whole milk, milkshakes and nutritional supplements.
Unless fat-containing foods or fluids clearly make you symptoms worse, fat should not be limited. This is because fats, particularly in liquids, provide a good source of calories in smaller, more manageable amounts.

Eating fibre is important to maintain bowel movements and overall gut health. Unless fibre-containing foods clearly make your symptoms worse, fibre should not be limited. If you identify high fibre foods that increase your symptoms, a dietitian can discuss suggestions to make sure you get enough fibre. Blending or liquidising meals that contain fibre may be helpful.
The foods that cause symptoms may vary from person to person. Because of this, it may be useful to keep a food and symptoms diary for a week to identify the foods that cause symptoms for you.

If eating smaller, more frequent meals does not improve your symptoms, the next step could be to try changing the texture of your foods.
Foods with a softer texture may empty out of the stomach more easily than solids. Simple measures such as properly chewing food may help if symptoms are mild. At mealtimes practice putting your fork down between mouthfuls, give each bite 20 chews and take 20 minutes to finish your meal. Sitting at the table rather than on the sofa would also be helpful.
Some softer meal ideas could include:

If you continue to struggle with symptoms, you may need pureed or liquid meals. Any of the soft meal options can be liquidised, but they may need to be thinned out with extra liquid.
Sweet or savoury liquids you could use include:
Savoury
Broths or soup
Water or stock
Milk - full fat or skimmed
Gravy
Tomato juice or passata
Sweet
Fruit Juice
Juice from tinned fruit
Condensed or evaporated milk
Plant based milk such as oat, soya or rice
Full fat or low-fat plain yogurt
If you chew gum, you may be swallowing air, causing bloating. Fizzy drinks will do the same. The polyol sweetener in gum and sugar free sweets can also cause stomach ache. See if avoiding gum and choosing still drinks reduces bloating, burping and pain.
Some people are also sensitive to caffeine in tea, coffee and energy drinks which may cause you to feel sick. Wean yourself off caffeine slowly as doing this too quickly can cause headaches.
Alcohol can slow down stomach emptying and worsen your symptoms.

It can sometimes be difficult to eat enough to maintain your weight. Higher energy foods and drinks can help meet your energy needs, without making the portion too big to manage.
Some ways to add an extra 100kcal to your meals include:

Nourishing drinks can also help support your energy needs, especially if you are only managing liquids.
Some ways to add an extra 100kcal to your meals include:
3-4 tablespoons of milk powder can be added to 500ml or 1 pint of milk to add extra nutrition. This can then be used in drinks and meals throughout the day to add extra calories.

Nutritional supplements can be a useful tool to make sure you get all the energy and protein your body needs. Supermarkets and chemists have supplements in sweet and savoury flavours which include Complan and Ensure. Other prescribed options are also available which you can discuss with your dietitian or doctor.
It can be helpful to agree a weight that you don’t want to fall under with your dietitian. This is to monitor progress. Please refer to the QR code card you were given if you chose to receive this information digitally.
If you notice your weight has dropped below the agreed lowest weight, you should contact your dietetic team. (Bradford Hospitals Nutrition and Dietetic Department: 01274 365108).

If you have diabetes, it is important to have good glucose control. Gastroparesis may make your food intake very variable. So, blood glucose levels can be harder to keep stable throughout the day. Many people find good blood glucose control helps to improve symptoms and similarly improved symptoms helps blood glucose levels.
Try to have similar amounts of carbohydrate at each meal whether its liquid or solid food.
If you monitor your blood glucose levels, you may need to glucose test more often.
If you dose adjust insulin for carbohydrate go through this with your dietitian to check your calculations are working and discover any new tools there may be to help.
When your gut is not working properly you may struggle with more hypos and they may be more difficult to treat. Please mention this to your care team if you are experiencing problems.
Your dietitian or diabetes team will help you make individualised dietary adjustments that suit your blood glucose management.

www.bradfordhospitals.nhs.uk/nutrition-and-dietetic Email: Dietitians.office@bthft.nhs.uk
Telephone: 01274 365108 between 8.30am and 4.30pm (answerphone available outside these hours).
You can contact us using the Relay UK app. Textphone users will need to dial 18001 ahead of the number to be contacted.