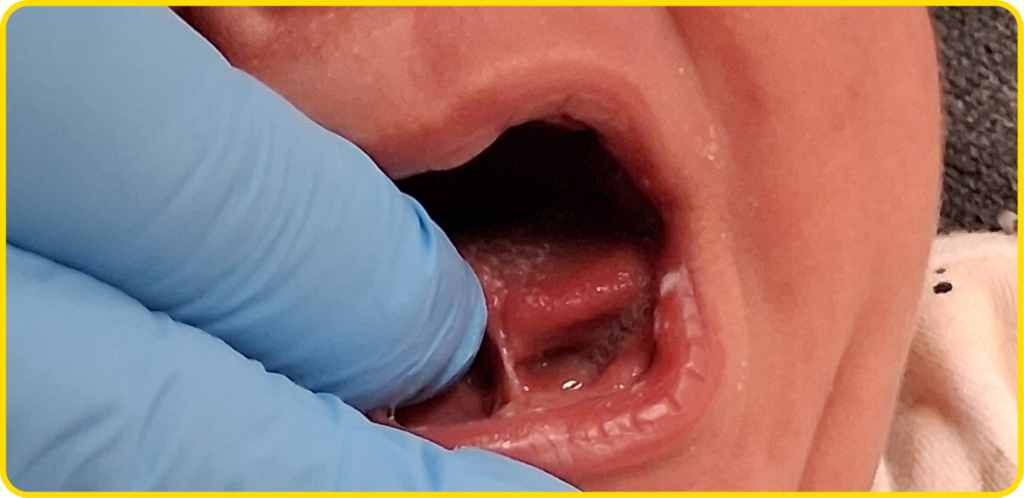
One in ten babies are born with a tongue-tie, which is also known as ankyloglossia. (pronounced ang-kuh-low-GLOSS-ee-uh). This is when the membrane under the tongue, the lingual frenulum, is shortened or tight and restricts the tongue’s movement and function.
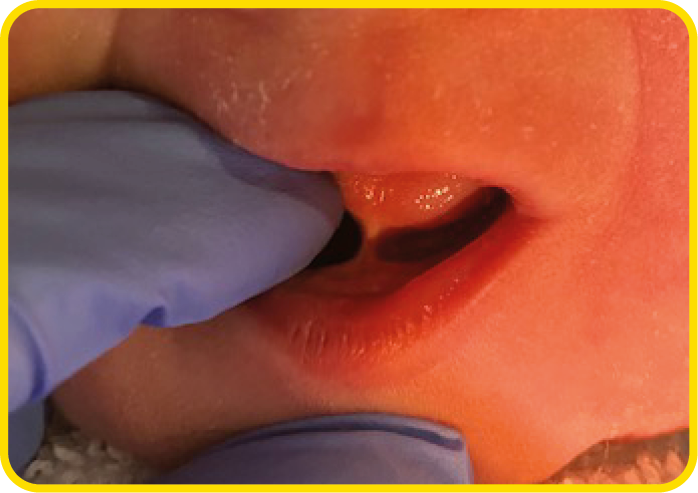
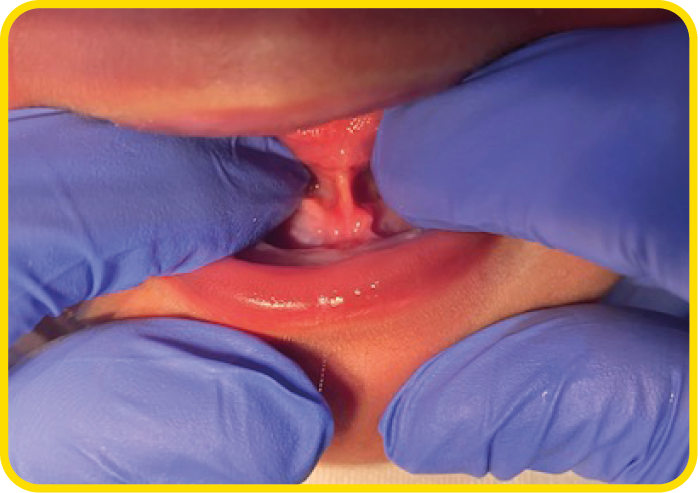
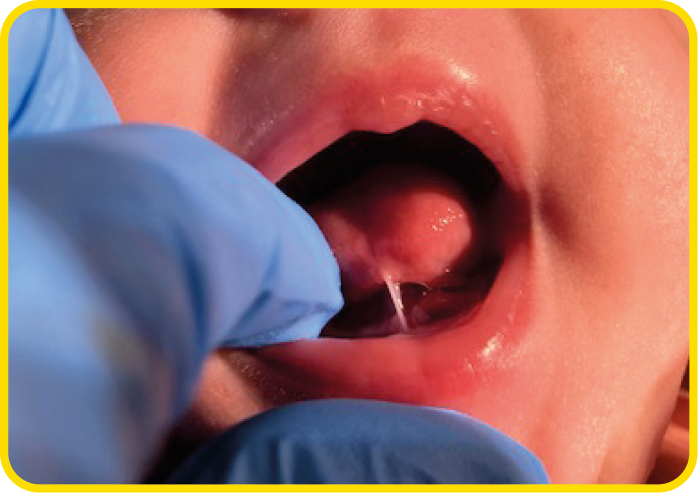
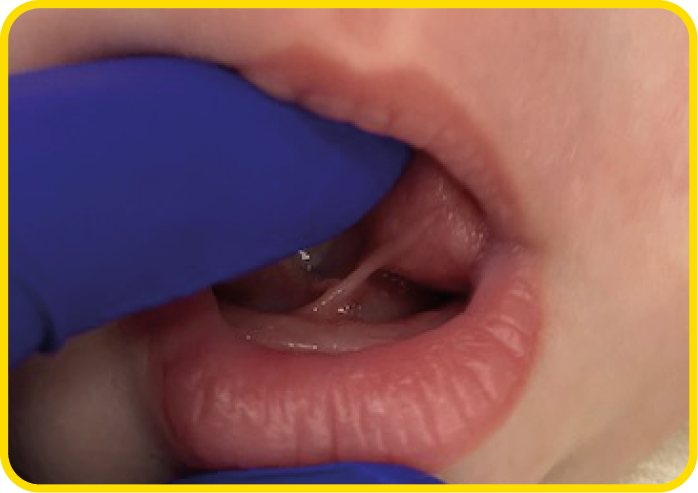
If the frenulum is attached at, or close to the tongue tip, the tongue may look blunt, forked, or be heart-shaped.
If the frenulum attaches closer to the base of the tongue, it may be easier to feel the restriction and requires an assessment of tongue function in more detail by an infant feeding specialist.
Infant’s Symptoms
Maternal Symptoms
Infant’s Symptoms
Maternal Symptoms
You and your baby may not have all these problems and there may be other reasons for the symptoms your baby has. It is important that you and your baby are assessed by the specialists in the Maternity Infant Feeding Team who are skilled in infant feeding support. Many infant feeding issues can be solved by changes to feeding methods. In addition to specialist feeding support, referral to body workers, such as osteopaths, may help with other issues such as tension which could be causing or contributing to these problems. During an infant feeding appointment, as part of the care provision, we can signpost you to these services.
If your baby still has problems despite specialist support, then the tongue-tie can be surgically released to improve tongue function and mobility. This procedure is called a Frenulotomy and is a simple surgery which usually involves cutting the frenulum with sharp, blunt-ended scissors. Anaesthetic or stitches are not usually needed, and the baby can breast or bottle feed straight after the procedure.
Complications are very rare, but include a lot of bleeding, infection, damage to the tongue and surrounding structures and scar tissue that may need additional surgery. Your tongue-tie practitioner will discuss the risk factors with you so you can make an informed choice.
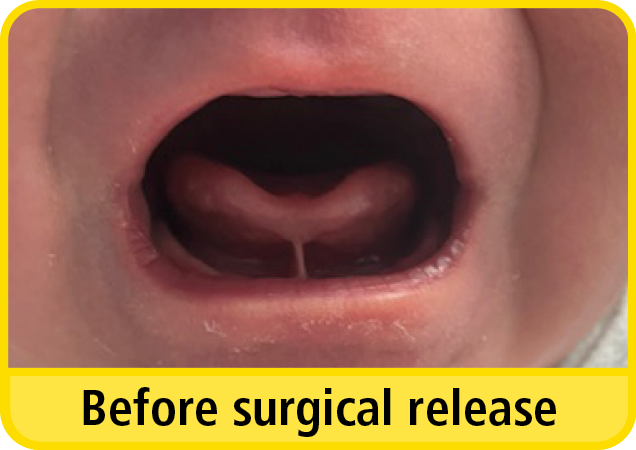
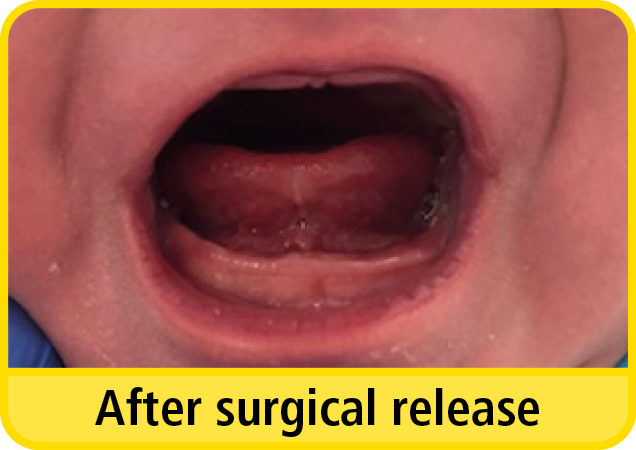
After the tongue-tie release, there may be a diamond shaped wound under the tongue. This will heal by itself, and you do not need to touch it. The appearance of the wound will be pink in colour to begin with, then over the first few days, it is normal for the wound to turn a white or yellow colour. If your baby is jaundiced at the time of the procedure, the wound may look a bright yellow or orange in colour.
The wound will get smaller and then disappear 7-14 days after the procedure.
Take extra care to fully sterilise any feeding equipment being used to reduce the risk of infection. All artificial milk feeds should be made up according to the manufacturer’s instructions on the packaging or, as per directions on Infant milks for parents & carers — First Steps Nutrition Trust.
For more information please visit:
https://www.firststepsnutrition.org/parents-carers
If you baby’s wound looks swollen, red and inflamed, or if your baby develops a temperature, reluctance to feed, is sleepy or irritable, please make an appointment with your GP or speak to the out of hours service or 111. Although it is very unlikely, your baby may need antibiotics. If you have questions about the wound healing, please contact the Maternity Infant Feeding Team on 01274 364583 to discuss or send an image of the wound.
Your practitioner will check your baby’s wound after the first feed to make sure all bleeding has stopped. If your baby vomits after the procedure, you may notice some pinkness in the milk or vomit. You may notice a streak of blackness in your baby’s stool later. This is due to a small amount of blood that may have been swallowed after the procedure.
Offer your baby the breast or a bottle of milk and feed them. This will usually stop the bleeding within a few minutes in the same way it did straight after the procedure. If your baby refuses to feed giving them a dummy, pacifier, or your clean finger will have a similar effect.
If the bleeding is very heavy, or it doesn’t reduce with feeding and stop within 15 minutes, then apply pressure to the wound under the tongue with one finger. Use a clean piece of gauze or muslin for 10 minutes. Do not apply pressure under your baby’s chin as this can affect their breathing.
If the bleeding continues after this time, and you are concerned, continue to apply pressure to the wound and call 999 to get your baby checked in hospital.
For more information please visit:
https://www.tongue-tie.org.uk/bleeding-guidelines
Babies react differently after the procedure. After their first feed, many babies sleep for a period of time due to the surge of adrenaline when they have the procedure. They then may become more unsettled and may be fussy with feeding for a day or so.
There are occasions where the wound heals so well, that the scar tissue forms with a restriction that can have the same effect on feeding as before the procedure, If you do notice a marked deterioration 4 weeks after the procedure, please contact the Maternity Infant Feeding Team to discuss this further on 01274 364583. They are available Monday – Friday between 8.30am until 4.00pm this does not include bank holidays.
All babies are different. You may notice your baby’s feeding technique improves immediately or, more likely, it may take time as you both get used to their more mobile tongue and adjust your position and attachment. Remember, you have been managing for a time with the tongue-tie, so both you and your baby may need to re-learn.
If your nipples were sore before the procedure, it may take some time for them to heal. In some cases, no notable improvement in feeding is observed. Do access the ongoing help you need.
Your tongue-tie practitioner will provide this or they will direct you to your most appropriate local services.
There is no evidence that wound massage or stretching works. However, with clean fingers and short nails, there are some gentle exercises you may wish to do to help tongue function to improve, in addition to frequent feeding:
This includes treatment of osteopathy, cranio-sacral therapy provided by a trained professional and can complement the effect of tongue-tie release to help with jaw or neck tightness and associated issues. These are services you access outside of the NHS but the Infant Feeding Team can signpost you.
You can contact us using the Relay UK app. Textphone users will need to dial 18001 ahead of the number to be contacted.
Bradford Teaching Hospitals NHS Foundation Trust is a smoke-free organisation. You are not permitted to smoke or in use e-cigarettes in any of the hospital buildings or grounds.